
India Insurance Third Party Administrator Market Size, Share, Trends and Forecast by Insurance Type, and Region, 2026-2034
India Insurance Third Party Administrator Market Summary:
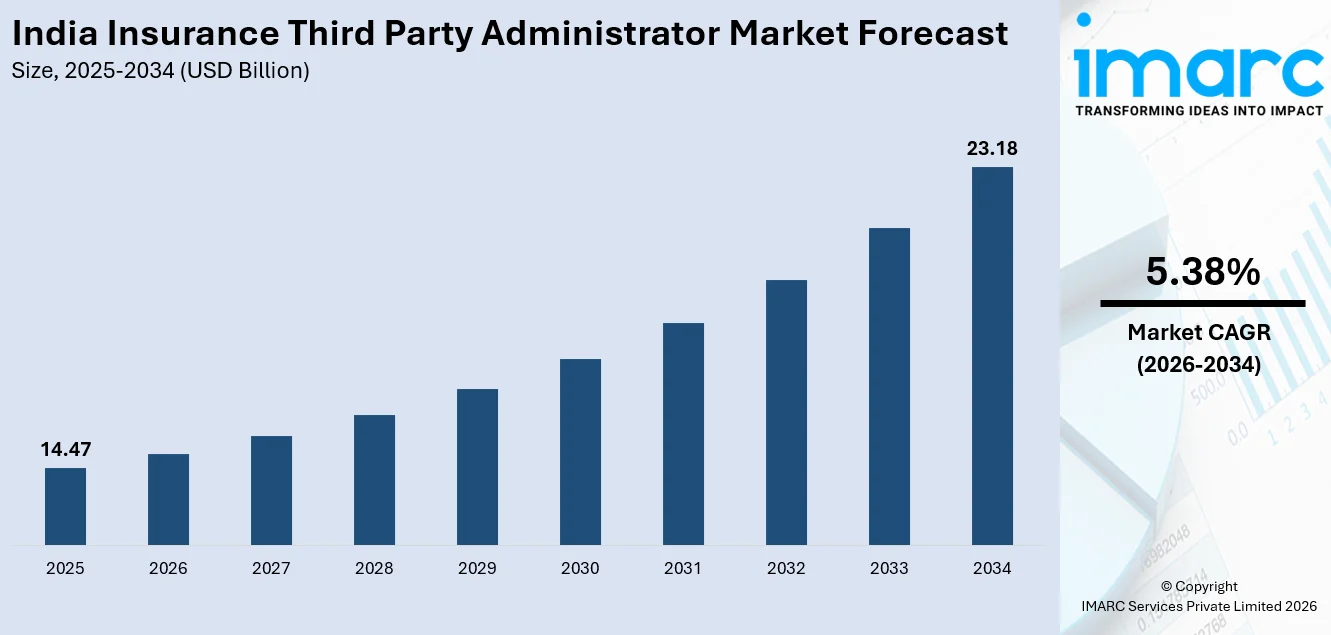
The India insurance third party administrator market size was valued at USD 14.47 Billion in 2025 and is projected to reach USD 23.18 Billion by 2034, growing at a compound annual growth rate of 5.38% from 2026-2034.
The India insurance third party administrator market is experiencing robust expansion as the country’s insurance sector undergoes rapid digitization and regulatory modernization. Increasing health insurance penetration, driven by government-backed schemes and rising consumer awareness, is fueling demand for efficient claims administration services. Supportive regulatory frameworks, technological advancements in automation and artificial intelligence, and the growing complexity of insurance products are compelling insurers to rely on specialized third party administrators for streamlined operations, fraud detection, and enhanced policyholder experiences, thereby strengthening the India insurance third party administrator market share.
Key Takeaways and Insights:
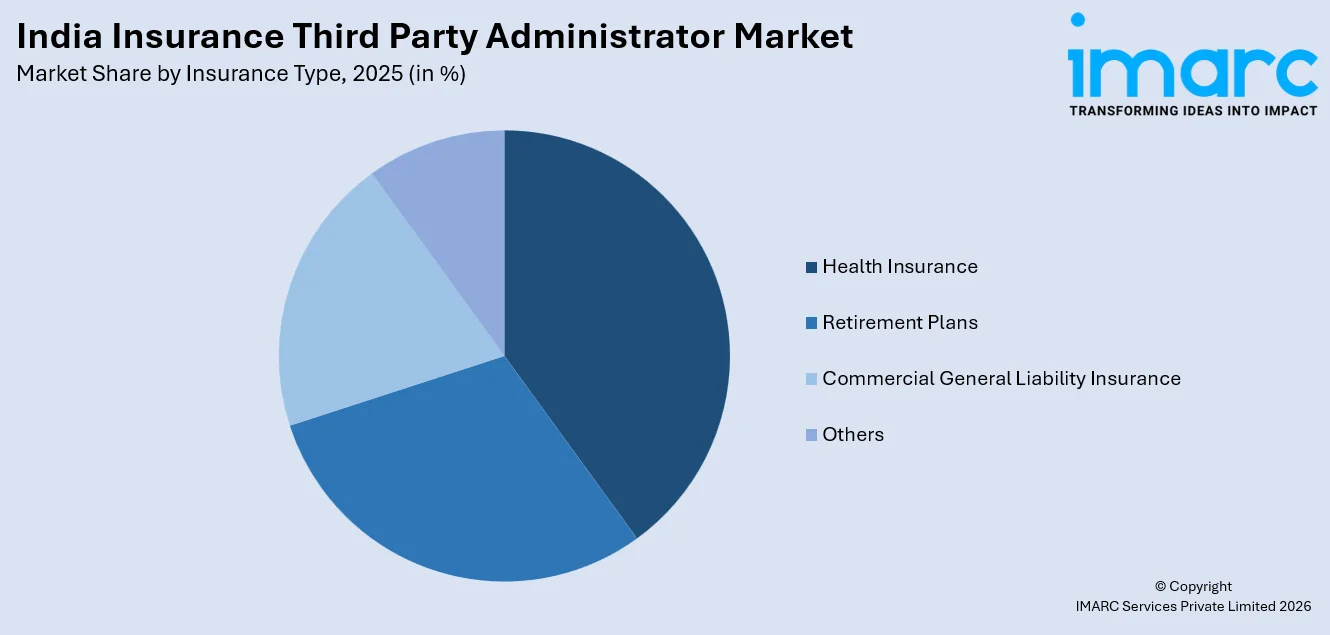
- By Insurance Type: Health insurance dominates the market with a share of 38% in 2025, driven by expanding government health coverage schemes, rising hospitalization rates, and increasing demand for cashless claim settlement services across the country.
- Key Players: The India insurance third party administrator market features a moderately consolidated competitive landscape, with established players strengthening market positions through strategic acquisitions, technology-driven service enhancements, and expanded insurer partnerships, while smaller TPAs compete on regional expertise and specialized service offerings.
To get more information of this market Request Sample
The India insurance third party administrator market is evolving rapidly as insurers increasingly outsource claims processing, policy administration, and customer service functions to specialized intermediaries. The sector is being reshaped by regulatory reforms from the Insurance Regulatory and Development Authority of India (IRDAI), which mandate greater transparency, faster claim settlements, and digital interoperability across the insurance value chain. In September 2024, the Union Cabinet approved the expansion of Ayushman Bharat PM-JAY to cover all senior citizens aged 70 years and above regardless of income, benefiting approximately six crore senior citizens across 4.5 crore families with free health coverage of up to INR five lakh per family annually. This expansion has substantially increased claim volumes, driving greater reliance on TPAs for efficient processing and administration. Concurrently, the integration of artificial intelligence, cloud-based platforms, and the National Health Claims Exchange is transforming operational efficiency and positioning TPAs as critical pillars of India’s insurance ecosystem.
India Insurance Third Party Administrator Market Trends:
Accelerated Digital Transformation and AI-Driven Claims Processing
The India insurance TPA sector is undergoing significant digital transformation as companies adopt artificial intelligence, machine learning, and cloud-based platforms to enhance claims adjudication and fraud detection capabilities. Digital pre-authorization systems and mobile applications are reducing turnaround times and improving policyholder transparency. For instance, in September 2025, IRDAI launched the Bima Sugam portal, a unified digital insurance marketplace designed to integrate all insurers, TPAs, and intermediaries on a single platform, enabling standardized digital transactions and accelerating the India insurance third party administrator market growth.
Industry Consolidation Through Strategic Mergers and Acquisitions
The TPA landscape in India is witnessing increased consolidation as larger players acquire smaller firms to expand market presence, strengthen insurer partnerships, and integrate advanced technology capabilities. This trend is driven by the need for scalable operations, improved service delivery, and enhanced automation. For instance, in August 2024, Medi Assist Insurance TPA signed a definitive agreement to acquire Paramount Health Services and Insurance TPA at an enterprise value of INR 311.18 crore, increasing its market share to 36.6% in the group segment and 23.6% of the overall health insurance industry by premiums managed.
Integration with National Health Claims Exchange for Interoperability
TPAs are actively integrating with the National Health Claims Exchange (NHCX), a collaborative initiative by the National Health Authority and IRDAI, to standardize and digitize health insurance claims processing across India. This integration facilitates seamless data exchange between insurers, hospitals, and TPAs, enabling faster claim settlements and reduced administrative costs. For instance, in November 2024, MDIndia Health Insurance TPA successfully processed its first claim through the NHCX platform, adopting the FHIR (Fast Healthcare Interoperability Resources) standard for uniform data formatting and real-time claim status tracking across the healthcare ecosystem.
Market Outlook 2026-2034:
The India insurance third-party administrator market is expected to witness steady expansion in the coming years, driven by rising insurance awareness, evolving regulatory frameworks, and increasing digitalization across the insurance value chain. Efforts to broaden healthcare access and strengthen policyholder protection are creating a favorable operating environment for TPAs. At the same time, regulatory emphasis on technology integration and system interoperability is enhancing process efficiency and transparency, thereby expanding growth opportunities and reinforcing the long-term relevance of TPA services within the health insurance ecosystem. The market generated a revenue of USD 14.47 Billion in 2025 and is projected to reach a revenue of USD 23.18 Billion by 2034, growing at a compound annual growth rate of 5.38% from 2026-2034.
India Insurance Third Party Administrator Market Report Segmentation:
| Segment Category | Leading Segment | Market Share |
|---|---|---|
|
Insurance Type |
Health Insurance |
38% |
Insurance Type Insights:
Access the comprehensive market breakdown Request Sample
- Health Insurance
- Retirement Plans
- Commercial General Liability Insurance
- Others
Health insurance dominates the market with a share of 38% of the total India insurance third party administrator market in 2025.
Health insurance constitutes the dominant segment of the India insurance TPA market, supported by increasing hospitalization trends and broader healthcare coverage initiatives. Rising awareness of preventive care and the growing burden of chronic conditions are contributing to higher claim frequencies, prompting insurers to depend on TPAs for streamlined claims processing, hospital network management, and customer support services. Ongoing efforts to widen public health coverage, particularly for senior citizens, are further elevating claim volumes and reinforcing the critical role of TPAs in administering and managing health insurance operations efficiently.
The segment is further bolstered by IRDAI’s regulatory reforms that mandate faster cashless claim approvals, reduced waiting periods for pre-existing diseases, and enhanced digital interoperability through platforms such as the National Health Claims Exchange. These regulatory requirements have compelled TPAs to invest in advanced technology infrastructure, including AI-powered claims adjudication systems and digital pre-authorization tools, to meet the stringent service-level benchmarks. As of July 2024, approximately 34 insurers and TPAs were live on the NHCX platform with roughly 300 hospitals ramping up integration, reflecting the accelerating digital transformation of health insurance claims processing across the country.
Regional Insights:
- North India
- South India
- East India
- West India
North India represents a significant share of the TPA market, supported by a large population base, high concentration of healthcare facilities in metropolitan areas such as Delhi and its surrounding regions, and strong penetration of both public and private health insurance schemes across the territory.
South India is a key contributor to the market, driven by advanced healthcare infrastructure, higher insurance awareness among consumers, and the presence of major technology hubs that facilitate the adoption of digital claims processing and policyholder management solutions.
East India presents emerging growth opportunities for TPAs, supported by expanding government-backed health insurance coverage, increasing healthcare accessibility in previously underserved areas, and rising awareness about the benefits of structured insurance administration services.
West India holds a prominent position in the market, anchored by the concentration of major insurance companies and TPA headquarters in Mumbai, robust corporate insurance demand from industrial corridors, and well-established hospital networks facilitating efficient cashless claim settlements.
Market Dynamics:
Growth Drivers:
Why is the India Insurance Third Party Administrator Market Growing?
Expanding Health Insurance Penetration Through Government Initiatives
The government’s strong emphasis on advancing universal health coverage is reshaping the insurance ecosystem and increasing reliance on third-party administrators. Broad-based public health programs are leading to a sharp rise in claim activity, necessitating efficient processing, verification, and settlement mechanisms. The continued expansion of national health protection initiatives, particularly those extending coverage to senior citizens, is widening the beneficiary base and deepening insurance penetration across vulnerable populations. As more individuals gain access to cashless treatment benefits, the operational role of TPAs becomes increasingly critical in managing high claim volumes, coordinating hospital networks, and ensuring timely reimbursements within the public health insurance framework.
Regulatory Reforms Mandating Digital Infrastructure and Service Standards
IRDAI’s comprehensive regulatory overhaul is compelling TPAs to upgrade their operational capabilities and invest in advanced digital infrastructure, thereby strengthening the overall market ecosystem. New regulations introduced in 2024 require insurers to approve cashless authorization requests within one hour and provide final authorization within three hours of receiving discharge requests, creating binding service-level benchmarks that necessitate sophisticated TPA technology platforms. Additionally, IRDAI launched the Bima Sugam portal in September 2025 as a unified digital insurance marketplace integrating all insurers, TPAs, and intermediaries on a single platform, with its first transactional phase scheduled for December 2025. These regulatory mandates are accelerating technology adoption and professionalization across the TPA sector, strengthening operational standards and policyholder service quality.
Rising Healthcare Costs and Growing Demand for Outsourced Administration
The escalating cost of healthcare in India, combined with the increasing complexity of insurance products and regulatory requirements, is driving insurers to outsource administrative functions to specialized TPAs. Rising hospitalization expenses, expanding treatment coverage mandates, and growing policyholder expectations for seamless digital experiences are placing significant operational demands on insurance companies. Health insurance premium collections in India have been registering consistent growth, leading to a corresponding rise in claim volumes that require efficient third-party administration. As product offerings become increasingly diversified and regulatory standards grow more rigorous, insurers are placing greater reliance on TPAs to manage operational complexities. Administrators equipped with advanced digital platforms, broad hospital networks, and specialized industry expertise are emerging as essential partners in enhancing process efficiency, compliance management, and overall service quality within the health insurance ecosystem.
Market Restraints:
What Challenges the India Insurance Third Party Administrator Market is Facing?
Stringent and Evolving Regulatory Compliance Requirements
The regular changes in the regulatory framework of IRDAI, which involve the guidelines on cashless operations, data migration protocols, and service-level benchmarks, are very costly to comply with by TPAs. All these needs require ongoing technology upgrades and a professional workforce, which exerts pressure on smaller TPAs and restricts their capacity to be flexible in their operations and innovative in their efforts.
Growing Trend of In-House Claims Management by Insurers
Some of the insurance companies are also building in-house claims processing capacity and creating established in-house health administration units. The trend decreases the use of external TPAs and limits the market that can be served, with insurers using proprietary technology platforms and direct hospital relationships to process claims without the use of intermediaries.
Data Security and Privacy Concerns in Digital Ecosystems
The growing number of digitalisation of claims and management of policyholder data and information puts the TPA at risk of more data privacy issues and enhanced cybersecurity threats. Since TPAs deal with highly personal health-related information and financial data, any serious data protection models and the implementation of smooth digital interoperability involve high costs and continue to be complicated to maintain processes.
Competitive Landscape:
The India insurance third party administrator market is characterized by a moderately consolidated competitive structure, with a few dominant players commanding significant market share alongside numerous smaller regional operators. Leading TPAs are pursuing aggressive expansion strategies through acquisitions, technology investments, and expanded insurer partnerships to strengthen their competitive positions. Competition is intensifying around service quality, digital capabilities, claims processing speed, and the breadth of hospital network coverage. Companies that effectively integrate artificial intelligence, automation, and data analytics into their operations are gaining competitive advantages, while smaller TPAs differentiate themselves through specialized regional expertise and personalized service delivery models.
Recent Developments:
- June 2024: Bajaj Allianz General Insurance conducted a workshop in Pune to promote hospital integration with the NHCX platform. This initiative supports digital claims processing adoption, fraud reduction, and greater transparency in health insurance settlements across the TPA industry.
- July 2024: The Health Ministry informed the Lok Sabha that, as of July 21, thirty-four insurers and Third-Party Administrators (TPAs) successfully onboarded onto the National Health Claims Exchange (NHCX) platform. The Ministry further noted that nearly 300 hospitals are in advanced stages of integration and are preparing to commence claim submissions through the digital exchange system, marking continued progress in the nationwide rollout of standardized electronic claims processing.
India Insurance Third Party Administrator Market Report Coverage:
| Report Features | Details |
|---|---|
| Base Year of the Analysis | 2025 |
| Historical Period | 2020-2025 |
| Forecast Period | 2026-2034 |
| Units | Billion USD |
| Scope of the Report |
Exploration of Historical Trends and Market Outlook, Industry Catalysts and Challenges, Segment-Wise Historical and Future Market Assessment:
|
| Insurance Types Covered | Health Insurance, Retirement Plans, Commercial General Liability Insurance, Others |
| Regions Covered | North India, South India, East India, West India |
| Customization Scope | 10% Free Customization |
| Post-Sale Analyst Support | 10-12 Weeks |
| Delivery Format | PDF and Excel through Email (We can also provide the editable version of the report in PPT/Word format on special request) |
Key Questions Answered in This Report
The India insurance third party administrator market size was valued at USD 14.47 Billion in 2025.
The India insurance third party administrator market is expected to grow at a compound annual growth rate of 5.38% from 2026-2034 to reach USD 23.18 Billion by 2034.
Health insurance, holding the largest share of 38% in 2025, is the dominant segment driven by expanding government health coverage programs, rising hospitalization volumes, growing demand for cashless claim services, and increasing consumer health awareness across India.
Key factors driving the India insurance third party administrator market include expanding health insurance penetration through government initiatives, regulatory reforms mandating digital infrastructure, rising healthcare costs, growing outsourcing of claims administration, and increasing adoption of AI-driven technology solutions.
Major challenges include stringent and frequently evolving IRDAI regulatory compliance requirements, the growing trend of insurers developing in-house claims management capabilities, data security and privacy concerns in digital ecosystems, and competitive pressures from market consolidation.
Need more help?
- Speak to our experienced analysts for insights on the current market scenarios.
- Include additional segments and countries to customize the report as per your requirement.
- Gain an unparalleled competitive advantage in your domain by understanding how to utilize the report and positively impacting your operations and revenue.
- For further assistance, please connect with our analysts.
 Request Customization
Request Customization
 Speak to an Analyst
Speak to an Analyst
 Request Brochure
Request Brochure
 Inquire Before Buying
Inquire Before Buying




.webp)




.webp)












