
Insurance Third Party Administrator Market Report by Insurance Type (Health Insurance, Retirement Plans, Commercial General Liability Insurance, and Others), and Region 2026-2034
Market Overview:
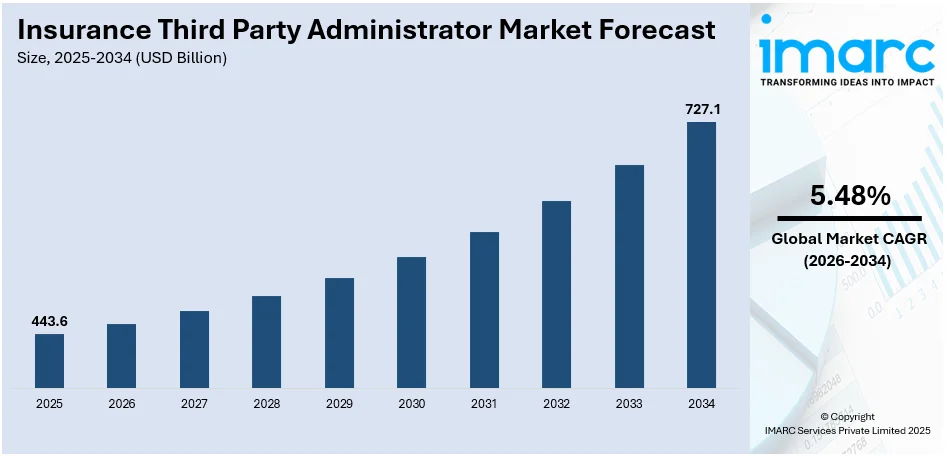
The global insurance third party administrator market size reached USD 443.6 Billion in 2025. Looking forward, IMARC Group expects the market to reach USD 727.1 Billion by 2034, exhibiting a growth rate (CAGR) of 5.48% during 2026-2034. The increasing demand for insurance TPA for complex claims handling, the rising utilization for risk mitigation, the growing integration with insurers' tech systems for efficient data sharing, and the escalating demand for streamlined administrative services are some of the factors propelling the market.
|
Report Attribute
|
Key Statistics |
|---|---|
|
Base Year
|
2025 |
|
Forecast Years
|
2026-2034
|
|
Historical Years
|
2020-2025
|
| Market Size in 2025 | USD 443.6 Billion |
| Market Forecast in 2034 | USD 727.1 Billion |
| Market Growth Rate (2026-2034) | 5.48% |
An insurance third party administrator is an intermediary that manages various aspects of insurance policies on behalf of insurance companies. It provides claims processing, policy administration, premium collection, and customer support services. It bridges the gap between insurers and policyholders, streamlining operations and improving efficiency. TPAs play a crucial role in simplifying the claims process. They assess claims, verify information, and facilitate prompt payments to beneficiaries. This speeds up the resolution process and enhances customer satisfaction. Additionally, TPAs handle policy administration tasks like issuing policies, endorsements, and renewals, reducing administrative burdens for insurers. By outsourcing these functions to TPAs, insurance companies can focus on underwriting, risk assessment, and expanding their business. Policyholders benefit from a smoother claims experience and more efficient service.
To get more information on this market Request Sample
The global market is majorly driven by the increasing complexities in insurance operations. In line with this, insurers seek cost-effective ways to manage administrative tasks, fueling TPA demand. Furthermore, the evolving regulations require expert handling, boosting TPA utilization. Apart from this, rapid technological advancements are offering numerous opportunities for the market. Moreover, the growing focus on core activities is catalyzing the market. Besides, the escalating competition prompts insurers to enhance service quality through TPAs, propelling the market. Additionally, the rising health coverage leads to increased TPA demand for claims processing.
Insurance Third Party Administrator Market Trends/Drivers:
Increasing operational outsourcing
The increasing trend of operational outsourcing is stimulating the market. Insurers are increasingly recognizing the value of delegating non-core functions to specialized TPAs. By entrusting tasks like claims processing, policy administration, and customer service to TPAs, insurers can optimize their resources and focus on core activities such as underwriting and risk assessment. This shift enhances operational efficiency, reduces administrative overhead, and allows insurers to respond more effectively to market dynamics. Operational outsourcing to TPAs also enables insurers to access expertise and technologies that might be cost-prohibitive to develop in-house. As the complexity of insurance operations increases and regulatory compliance becomes more intricate, TPAs provide a dedicated approach to managing these challenges. This strategic collaboration fosters a competitive edge for insurers, enhances customer experience, and accelerates growth in the insurance industry.
Rising emphasis on fraud detection
The escalating emphasis on fraud detection is propelling the market. As insurance fraud becomes more sophisticated and prevalent, TPAs equipped with advanced fraud detection technologies and strategies offer insurers a potent solution to safeguard their operations. TPAs employ data analytics, artificial intelligence, and predictive modeling to identify fraudulent claims, reducing financial losses for insurers. By partnering with TPAs, insurers can tap into a pool of expertise focused on combating fraud. TPAs bring specialized resources, enabling insurers to adopt proactive measures that enhance risk assessment and prevent fraudulent activities. This collaborative approach mitigates financial losses and bolsters insurers' reputation for fair practices. As the insurance landscape navigates evolving risks, the integration of robust fraud detection through TPAs fuels industry growth by reinforcing trust, minimizing losses, and ensuring a secure operational environment.
Growing demand for digital transformation support
The increasing demand for digital transformation support is bolstering the market. Insurers recognize the imperative to modernize their operations through digitization, and TPAs are valuable partners in this endeavor. TPAs offer specialized knowledge and technological infrastructure that facilitate seamless digital integration, enabling insurers to optimize processes, enhance customer experiences, and stay competitive in a rapidly evolving landscape. TPAs assist insurers in implementing digital tools, such as automated claims processing, online policy management, and customer self-service portals. Their expertise aids in navigating the complexities of digital adoption, reducing implementation time and potential hiccups. By leveraging TPAs for digital transformation, insurers can swiftly adapt to changing consumer preferences and industry trends. This collaborative synergy between TPAs and insurers fosters growth by positioning the industry to capitalize on the vast opportunities presented by the digital revolution.
Insurance Third Party Administrator Industry Segmentation:
IMARC Group provides an analysis of the key trends in each segment of the global insurance third party administrator market report, along with forecasts at the global, the regional and country levels from 2026-2034. Our report has categorized the market based on insurance type.
Breakup by Insurance Type:
Access the comprehensive market breakdown Request Sample
- Health Insurance
- Retirement Plans
- Commercial General Liability Insurance
- Others
Health insurance dominates the market
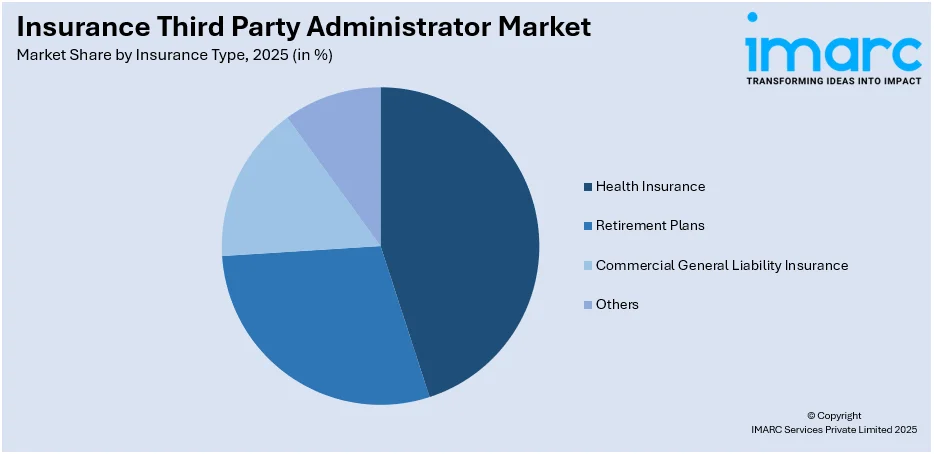
The report has provided a detailed breakup and analysis of the market based on the insurance type. This includes health insurance, retirement plans, commercial general liability insurance, and others. According to the report, health insurance represented the largest segment.
In health insurance, TPAs offer multiple services, such as claims processing, provider network management, and member services. Health insurance has witnessed a surge in demand due to increased healthcare awareness, regulatory changes, and aging populations. TPAs cater to these trends by providing efficient claims management, enabling faster reimbursements and hassle-free interactions for policyholders and healthcare providers. As the health insurance landscape evolves with new policy offerings and benefits, TPAs remain vital partners in delivering streamlined administration and customer satisfaction.
Furthermore, retirement plans constitute another critical segment. They have gained immense importance with a growing focus on financial security and planning. TPAs are crucial in managing retirement accounts, ensuring compliance with regulations, facilitating contributions, and assisting in benefit disbursements. Their expertise helps employers offer attractive retirement packages while adhering to legal frameworks. As the workforce becomes more diverse and mobile, TPAs provide flexibility to accommodate changing retirement preferences and ensure smooth employee transitions.
Breakup by Region:
- North America
- United States
- Canada
- Europe
- Germany
- France
- United Kingdom
- Italy
- Spain
- Others
- Asia Pacific
- China
- Japan
- India
- South Korea
- Australia
- Indonesia
- Others
- Latin America
- Brazil
- Mexico
- Others
- Middle East and Africa
North America exhibits a clear dominance, accounting for the largest market share
The report has also provided a comprehensive analysis of all the major regional markets, which include North America (the United States and Canada); Europe (Germany, France, the United Kingdom, Italy, Spain, and others); Asia Pacific (China, Japan, India, South Korea, Australia, Indonesia, and others); Latin America (Brazil, Mexico, and others); and the Middle East and Africa. According to the report, North America holds the leading position in the market.
In North America, TPAs are witnessing increased demand due to complex regulatory landscapes, rising healthcare costs, and a need for streamlined administrative processes. With the intricacies of the U.S. healthcare system, TPAs play a crucial role in managing health insurance claims, provider networks, and member services. Additionally, focusing on retirement planning in North America further boosts TPA growth, as TPAs assist in efficiently administrating diverse retirement plans, including 401(k)s and pension plans.
Furthermore, the TPA market in Europe is flourishing as insurers grapple with varying regulations across countries and languages. TPAs bridge insurers and diverse local regulations, facilitating claims processing and policy management. The growing importance of data protection regulations, such as GDPR, adds to the demand for TPAs that can ensure compliance. Moreover, Europe's aging population drives the need for efficient retirement plan administration, where TPAs offer services to manage pension funds and ensure regulatory adherence.
Competitive Landscape:
Top companies are pivotal in driving and strengthening market growth through various strategic approaches. These companies leverage their extensive expertise, advanced technology infrastructure, and industry insights to enhance the overall value proposition for insurers. They focus on innovation by continually upgrading their technological capabilities. This includes implementing AI-driven claims processing, digital interfaces for policyholders, and data analytics for improved risk assessment. Such advancements enhance operational efficiency and improve customer experiences, attracting more insurers to their services. Furthermore, top TPAs prioritize compliance with changing regulations. Staying ahead of legal requirements ensures their clients can navigate complex compliance landscapes seamlessly, fostering trust and credibility among insurers and policyholders. Moreover, these companies offer specialized services tailored to insurance segments, from health to property and casualty. This niche expertise resonates with insurers seeking tailored solutions, further expanding their market reach. Additionally, these companies engage in strategic partnerships, collaborating with insurers and reinsurers to create synergistic solutions. By combining forces, they optimize services, reduce costs, and provide comprehensive offerings that appeal to a wider array of insurers.
The report has provided a comprehensive analysis of the competitive landscape in the insurance third party administrator market. Detailed profiles of all major companies have also been provided.
- Charles Taylor Plc
- Crawford & Company
- ESIS Inc.
- ExlService Holdings Inc
- Gallagher Bassett Services Inc
- Helmsman Management Services LLC
- Meritain Health (Aetna Inc)
- Sedgwick Claims Management Services Ltd
- United HealthCare Services, Inc
Insurance Third Party Administrator Market Report Scope:
| Report Features | Details |
|---|---|
| Base Year of the Analysis | 2025 |
| Historical Period | 2020-2025 |
| Forecast Period | 2026-2034 |
| Units | Billion USD |
| Scope of the Report | Exploration of Historical and Forecast Trends, Industry Catalysts and Challenges, Segment-Wise Historical and Predictive Market Assessment:
|
| Insurance Types Covered | Health Insurance, Retirement Plans, Commercial General Liability Insurance, Others |
| Regions Covered | North America, Europe, Asia Pacific, Latin America, Middle East and Africa |
| Countries Covered | United States, Canada, Germany, France, United Kingdom, Italy, Spain, China, Japan, India, South Korea, Australia, Indonesia, Brazil, Mexico |
| Companies Covered | Charles Taylor Plc, Crawford & Company, ESIS Inc., ExlService Holdings Inc, Gallagher Bassett Services Inc, Helmsman Management Services LLC, Meritain Health (Aetna Inc), Sedgwick Claims Management Services Ltd, United HealthCare Services, Inc. etc. |
| Customization Scope | 10% Free Customization |
| Post-Sale Analyst Support | 10-12 Weeks |
| Delivery Format | PDF and Excel through Email (We can also provide the editable version of the report in PPT/Word format on special request) |
Key Questions Answered in This Report:
- How has the global insurance third party administrator market performed so far, and how will it perform in the coming years?
- What are the drivers, restraints, and opportunities in the global insurance third party administrator market?
- What is the impact of each driver, restraint, and opportunity on the global insurance third party administrator market?
- What are the key regional markets?
- Which countries represent the most attractive insurance third party administrator market?
- What is the breakup of the market based on the insurance type?
- Which is the most attractive insurance type in the global insurance third party administrator market?
- What is the competitive structure of the global insurance third party administrator market?
- Who are the key players/companies in the global insurance third party administrator market?
Key Benefits for Stakeholders:
- IMARC’s report offers a comprehensive quantitative analysis of various market segments, historical and current market trends, market forecasts, and dynamics of the insurance third party administrator market from 2020-2034.
- The research study provides the latest information on the market drivers, challenges, and opportunities in the global insurance third party administrator market.
- The study maps the leading, as well as the fastest-growing, regional markets. It further enables stakeholders to identify the key country-level markets within each region.
- Porter's five forces analysis assists stakeholders in assessing the impact of new entrants, competitive rivalry, supplier power, buyer power, and the threat of substitution. It helps stakeholders to analyze the level of competition within the insurance third party administrator industry and its attractiveness.
- Competitive landscape allows stakeholders to understand their competitive environment and provides an insight into the current positions of key players in the market.
Need more help?
- Speak to our experienced analysts for insights on the current market scenarios.
- Include additional segments and countries to customize the report as per your requirement.
- Gain an unparalleled competitive advantage in your domain by understanding how to utilize the report and positively impacting your operations and revenue.
- For further assistance, please connect with our analysts.
 Request Customization
Request Customization
 Speak to an Analyst
Speak to an Analyst
 Request Brochure
Request Brochure
 Inquire Before Buying
Inquire Before Buying




.webp)




.webp)












